Table of Contents
I. What is Psoriatic Arthritis?
II. Symptoms of Psoriatic Arthritis
III. Risk Factors for Psoriatic Arthritis
What is Psoriatic Arthritis?
Psoriatic arthritis, also known as PsA, is a rheumatic disease. Rheumatic diseases involve any disorder that affect the ligaments, bones, muscles, and joint tendons. Psoriatic arthritis is one such disease that affects the joints as well as the skin. Over 1.5 million people in the United States have psoriatic arthritis. [1]
This type of arthritis differs from others because it often accompanies psoriasis. Psoriasis is an incurable skin disease that occurs in flare-ups throughout a person’s life. This painful condition leads to symptoms that often include:
- Dry, cracked skin
- Itching or burning sensation
- Red patches of skin
- Silvery scales on the inflamed skin
- Thickened or pitted nails
- Swollen and stiff joints [1]
Around one in three people with psoriasis will develop psoriatic arthritis. Psoriasis is an immunological disorder where the body attacks the immune system. This immune response causes inflammation and overproduction of skin cells. Psoriatic arthritis typically occurs several years after the onset of psoriasis. Read on to learn more about psoriatic arthritis and treatments like Arava. [2]
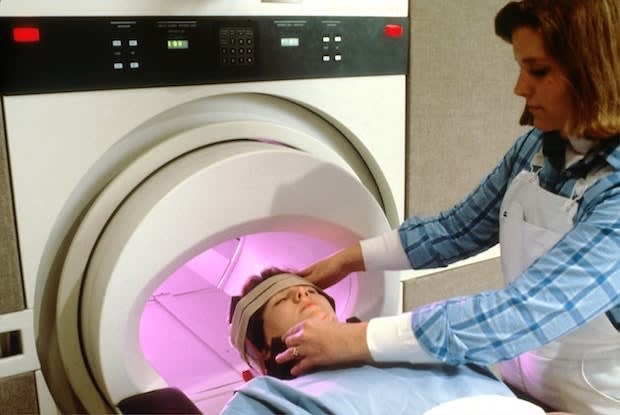
Having both psoriasis and psoriatic arthritis can take a toll on a person’s physical and mental health. Both of these conditions can have different symptoms and typically get worse as time goes on. The symptoms are often similar to rheumatoid arthritis, so you and your doctor must accurately determine your symptoms for proper diagnosis. The most common symptoms include: Foot pain: This type of arthritis affects the points in the foot where tendons and ligaments attach to the bones. Painful sensations occur most commonly at the back of the heel or the sole of the foot. Swollen Fingers and Toes: A swelling of the fingers and toes can deform the hands and feet. Your fingers and toes may develop a sausage-like appearance. Lower Back Pain: Back pain called spondylitis can occur along with psoriatic arthritis. Spondylitis is an inflammation of the joints between the spinal vertebrae. [3] The symptoms of psoriasis and psoriatic arthritis often overlap, so other symptoms can include: The exact cause of psoriatic arthritis is not known. As mentioned above, having psoriasis is a major risk factor, but it is not the only one. The following may play a major role in the development of psoriatic arthritis: Immunologic Causes: Psoriasis and psoriatic arthritis are caused by malfunctions in the immune symptoms. These conditions occur due to intense chronic inflammation. This disease targets skin cells, which begin to target joints, eyes, nails, and kidneys. Genetics: Psoriatic arthritis is often a genetic condition. Psoriatic arthritis is the result of malfunctioning T-cells in the body, which leads to chronic inflammation. These genes can be inherited, and you are 55 times more likely to get this disease if a parent or sibling also has it. [5] Lifestyle factors: There are several things you can do throughout your life that can contribute to your risk of psoriatic arthritis. One 2011 study by Harvard found that women who smoked were three times more likely to develop psoriatic arthritis than those who have never smoked. Past smokers were also found to be 50 percent more likely to get psoriatic arthritis. Along with smokers, obese people are at a higher risk for this joint disease. Psoriasis patients who are overweight are significantly more likely to develop psoriatic arthritis compared to those whose weight is normal. [5] Age: This condition can develop in anyone at any time but is more common in those between the ages of 30 and 50. On average, PsA develops five to 10 years after the development of psoriasis. [5] Prior conditions: Some research has shown that those who have previously had streptococcal infections have a greater chance of developing psoriasis and psoriatic arthritis. This link has not yet been fully proven. Psoriatic arthritis can also occur more frequently in those with a compromised immune system, especially HIV (human immunodeficiency virus). [5] If you already have psoriasis, your doctor will likely check in periodically to make sure you are not experiencing arthritis symptoms. If you start to notice creaky and sore joints, your doctor will do a thorough physical exam. During this exam, the doctor will press on the soles of your feet and heels, check your fingernails for pitting, and examine joints for signs of swelling. They may also order the following tests: X-rays: X-rays can be used to rule out any other causes behind sore and painful joints. They can also determine any damage to the joints caused by arthritis. MRI (magnetic resonance imaging): This test uses radio waves and a strong magnetic field to see if there are any problems in the tendons or ligaments in the feet or lower back. Joint Fluid Test: Your doctor will insert a needle into the painful joint and extract joint fluid. This fluid will be tested for uric acid crystals and indicate if you have gout or psoriatic arthritis. [6] Psoriatic arthritis can be a complicated condition to treat, especially if psoriasis is being treated simultaneously. To relieve minor pain, you can use NSAIDs (nonsteroidal anti-inflammatory drugs) like ibuprofen to reduce everyday inflammation. There are also immunosuppressant drugs like Neoral that can help those whose immune system is not working properly. Neoral (cyclosporine) can help the immune system from going into overdrive and causing severe inflammation. DMARDs, or disease-modifying antirheumatic drugs, can help slow the progression of psoriatic arthritis. With prolonged use, the joints can be saved from permanent damage. Arava (leflunomide) is one such DMARD that can improve the symptoms of this joint disease. Your doctor will determine the right medication plan for you. [6] The content in this article is intended for informational purposes only. This website does not provide medical advice. In all circumstances, you should always seek the advice of your physician and/or other qualified health professionals(s) for drug, medical condition, or treatment advice. The content provided on this website is not a substitute for professional medical advice, diagnosis or treatment.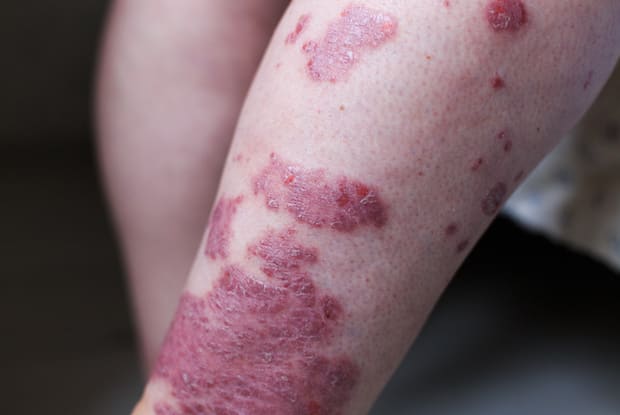
Symptoms of Psoriatic Arthritis
Risk Factors for Psoriatic Arthritis

Diagnosis
Treatment
